Introduction
Background
First described in 1922, Stevens-Johnson syndrome (SJS) is an immune-complex–mediated hypersensitivity complex that is a severe expression of erythema multiforme. It is known by some as erythema multiforme major, but disagreement exists in the literature. Most authors and experts consider Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN) different manifestations of the same disease. For that reason, many refer to the entity as SJS/TEN. SJS typically involves the skin and the mucous membranes. While minor presentations may occur, significant involvement of oral, nasal, eye, vaginal, urethral, GI, and lower respiratory tract mucous membranes may develop in the course of the illness. GI and respiratory involvement may progress to necrosis. SJS is a serious systemic disorder with the potential for severe morbidity and even death. Missed diagnosis is common.
Although several classification schemes have been reported, the simplest breaks the disease down as follows:1
- Stevens-Johnson syndrome - A "minor form of TEN," with less than 10% body surface area (BSA) detachment
- Overlapping Stevens-Johnson syndrome/toxic epidermal necrolysis (SJS/TEN) - Detachment of 10-30% BSA
- Toxic epidermal necrolysis - Detachment of more than 30% BSA
Pathophysiology
Stevens-Johnson syndrome is an immune-complex–mediated hypersensitivity disorder that may be caused by many drugs, viral infections, and malignancies. Cocaine recently has been added to the list of drugs capable of producing the syndrome. In up to half of cases, no specific etiology has been identified.
Pathologically, cell death results causing separation of the epidermis from the dermis. The death receptor, Fas, and its ligand, FasL, have been linked to the process. Some have also linked inflammatory cytokines to the pathogenesis.
Frequency
United States
Cases tend to have a propensity for the early spring and winter.
International
SJS occurs with a worldwide distribution similar in etiology and occurrence to that in the United States.
Mortality/Morbidity
- Mortality is determined primarily by the extent of skin sloughing. When BSA sloughing is less than 10%, the mortality rate is approximately 1-5%. However, when more than 30% BSA sloughing is present, the mortality rate is between 25% and 35%.2 See SCORTEN for a more complete discussion of severity of illness and mortality.
- Lesions may continue to erupt in crops for as long as 2-3 weeks. Mucosal pseudomembrane formation may lead to mucosal scarring and loss of function of the involved organ system. Esophageal strictures may occur when extensive involvement of the esophagus exists. Mucosal shedding in the tracheobronchial tree may lead to respiratory failure.
- Ocular sequelae may include corneal ulceration and anterior uveitis. Blindness may develop secondary to severe keratitis or panophthalmitis in 3-10% of patients. Vaginal stenosis and penile scarring have been reported. Renal complications are rare.
Race
A Caucasian predominance has been reported.
Sex
In Stevens-Johnson syndrome, the male-to-female ratio is 2:1.
Age
Most patients are in the second to fourth decade of their lives; however, cases have been reported in children as young as 3 months.
Clinical
History
- Typically, the disease process begins with a nonspecific upper respiratory tract infection.
- This usually is part of a 1- to 14-day prodrome during which fever, sore throat, chills, headache, and malaise may be present.
- Vomiting and diarrhea are occasionally noted as part of the prodrome.
- Mucocutaneous lesions develop abruptly. Clusters of outbreaks last from 2-4 weeks. The lesions are typically nonpruritic.
- A history of fever or localized worsening should suggest a superimposed infection; however, fever has been reported to occur in up to 85% of cases.
- Involvement of oral and/or mucous membranes may be severe enough that patients may not be able to eat or drink.
- Patients with genitourinary involvement may complain of dysuria or an inability to void.
- A history of a previous outbreak of Stevens-Johnson syndrome (SJS) or of erythema multiforme may be elicited. Recurrences may occur if the responsible agent is not eliminated or if the patient is reexposed.
- Typical symptoms are as follows:
- Cough productive of a thick purulent sputum
- Headache
- Malaise
- Arthralgia
Physical
- The rash can begin as macules that develop into papules, vesicles, bullae, urticarial plaques, or confluent erythema.
- The center of these lesions may be vesicular, purpuric, or necrotic.
- The typical lesion has the appearance of a target. The target is considered pathognomonic. However, in contrast to the typical erythema multiforme lesions, these lesions have only two zones of color. The core may be vesicular, purpuric, or necrotic; that zone is surrounded by macular erythema. Some have called these targetoid lesions.
- Lesions may become bullous and later rupture, leaving denuded skin. The skin becomes susceptible to secondary infection.
Note extensive sloughing of epidermis from Stevens-Johnson syndrome. Courtesy of David F. Butler, MD.
- Urticarial lesions typically are not pruritic.
- Infection may be responsible for the scarring associated with morbidity.
- Although lesions may occur anywhere, the palms, soles, dorsum of the hands, and extensor surfaces are most commonly affected.
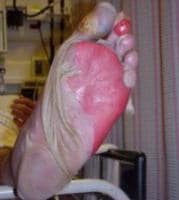
Sheetlike desquamation on the foot in a patient with toxic epidermal necrolysis. Courtesy of Robert Schwartz, MD.
- The rash may be confined to any one area of the body, most often the trunk.
- Mucosal involvement may include erythema, edema, sloughing, blistering, ulceration, and necrosis.
- Although some have suggested the possibility of Stevens-Johnson syndrome (SJS) without skin lesions, most believe that mucosal lesions alone are not enough to establish the diagnosis. Some are now calling cases without skin lesions "atypical" or "incomplete."3
- The following signs may be noted on examination:
- Fever
- Orthostasis
- Tachycardia
- Hypotension
- Altered level of consciousness
- Epistaxis
- Conjunctivitis
- Corneal ulcerations
- Erosive vulvovaginitis or balanitis
- Seizures, coma
Causes
- Drugs and malignancies are most often implicated as the etiology in adults and elderly persons.
- Pediatric cases are related more often to infections than to malignancy or a reaction to a drug.
- A medication such as sulfa, phenytoin, or penicillin had previously been prescribed to more than two thirds of all patients with Stevens-Johnson syndrome (SJS). The anticonvulsant oxcarbazepine (Trileptal) has also been implicated. Hallgren et al reported ciprofloxacin-induced Stevens-Johnson syndrome in young patients in Sweden and commented on several others.4 Metry et al reported Stevens-Johnson syndrome in 2 HIV patients treated with nevirapine and mentioned one other in the literature.5 The authors speculated that the problem may extend to other non-nucleoside reverse transcriptase inhibitors.5 Indinavir has been mentioned.
- More than half of the patients with Stevens-Johnson syndrome report a recent upper respiratory tract infection.
- The 4 etiologic categories are (1) infectious, (2) drug-induced, (3) malignancy-related, and (4) idiopathic.
- Viral diseases that have been reported include herpes simplex virus (HSV), AIDS, coxsackie viral infections, influenza, hepatitis, mumps, mycoplasmal infection, lymphogranuloma venereum (LGV),rickettsial infections, and variola.
- Bacterial etiologies include group A beta streptococci, diphtheria, Brucellosis, mycobacteria,Mycoplasma pneumoniae, tularemia, and typhoid. An "incomplete" case was recently reported afterMycoplasma pneumoniae infection.3
- Coccidioidomycosis, dermatophytosis, and histoplasmosis are the fungal possibilities.
- Malaria and trichomoniasis have been reported as protozoal causes.
- In children, Epstein-Barr virus and enteroviruses have been identified.
- Drug etiologies include penicillins and sulfa antibiotics. Anticonvulsants including phenytoin,carbamazepine, valproic acid, lamotrigine, and barbiturates have been implicated. Mockenhapupt et al stressed that most anticonvulsant-induced SJS occurs in the first 60 days of use.6 In late 2002, the US Food and Drug Administration (FDA) and the manufacturer Pharmacia noted that Stevens-Johnson syndrome (SJS) had been reported in patients taking the cyclooxygenase-2 (COX-2) inhibitor valdecoxib. In 2007, the US FDA reported SJS/TEN in patients taking modafinil (Provigil). Allopurinol has recently been implicated as the most common cause in Europe and Israel.7
- Various carcinomas and lymphomas have been associated.
- Stevens-Johnson syndrome (SJS) is idiopathic in 25-50% of cases
Differential Diagnoses
Burns, Chemical
Erythema Multiforme
Burns, Ocular
Staphylococcal Scalded Skin Syndrome
Burns, Thermal
Toxic Epidermal Necrolysis
Dermatitis, Exfoliative
Toxic Shock Syndrome
Other Problems to Be Considered
Acute generalized exanthematic pustulosis
Pemphigus
Workup
Laboratory Studies
- No specific laboratory studies (other than biopsy) exist that can definitively establish the diagnosis of Stevens-Johnson syndrome.
- A complete blood count (CBC) may reveal a normal white blood cell (WBC) count or a nonspecific leukocytosis. A severely elevated WBC count indicates the possibility of a superimposed bacterial infection.
- Determine renal function and evaluate urine for blood.
- Electrolytes and other chemistries may be needed to help manage related problems.
- Cultures of blood, urine, and wounds are indicated when an infection is clinically suspected.
- Bronchoscopy, esophagogastroduodenoscopy (EGD), and colonoscopy may be indicated.
Imaging Studies
- Chest radiography may indicate the existence of a pneumonitis when clinically suspected. Otherwise, routine plain films are not indicated.
Other Tests
- Skin biopsy is the definitive diagnostic study but is not an emergency department (ED) procedure.
- Skin biopsy specimens demonstrate that the bullae are subepidermal.
- Epidermal cell necrosis may be noted.
- Perivascular areas are infiltrated with lymphocytes.
Treatment
Prehospital Care
Paramedics should recognize the presence of severe fluid loss and should treat patients with Stevens-Johnson syndrome (SJS) as they would patients with thermal burns.
Emergency Department Care
Most patients present early and prior to obvious signs of hemodynamic compromise. The single most important role for the ED physician is to detect Stevens-Johnson syndrome/toxic epidermal necrolysis (SJS/TEN) early and initiate the appropriate ED and inpatient management.
Withdrawal of the suspected offending agent is critically important. Timing of withdrawal has been linked to outcome.
- Care in the ED must be directed to fluid replacement and electrolyte correction.
- Skin lesions are treated as burns.
- Patients with SJS/TEN should be treated with special attention to airway and hemodynamic stability, fluid status, wound/burn care, and pain control.
- Treatment is primarily supportive and symptomatic. Some have advocated cyclophosphamide, plasmapheresis, hemodialysis, and immunoglobulin. Most authorities believe that corticosteroids are contraindicated.
- Manage oral lesions with mouthwashes.
- Topical anesthetics are useful in reducing pain and allowing the patient to take in fluids.
- Areas of denuded skin must be covered with compresses of saline or Burow solution.
- Underlying diseases and secondary infections must be identified and treated. Offending drugs must be stopped.
- The use of systemic steroids is controversial. Some authors believe that they are contraindicated. Treatment with systemic steroids has been associated with an increased prevalence of complications.
- In a large European study designed to evaluate the efficacy of various treatments, the EuroSCAR Study "found no sufficient evidence of a benefit for any specific treatment."8 The group looked at mortality in patients treated with IV immunoglobulins and corticosteroids.
- Address tetanus prophylaxis.
Consultations
Consultants may help establish the diagnosis and direct inpatient care. A dermatologist is the most likely clinician to establish the diagnosis, with or without biopsy.
- Severe cases may require the involvement of a burn specialist or plastic surgery specialist.
- Internal medicine, critical care, or pediatrics consultants direct inpatient care.
- Ophthalmology consultation is mandatory for those with ocular involvement.
- Depending on organ system involvement, consultations with a gastroenterologist, pulmonologist, and nephrologist may be helpful.
Medication
No specific drug treatment has been consistently shown to be beneficial in the treatment of Stevens-Johnson syndrome. The choice of antibiotic depends on the associated infection. The use of systemic corticosteroids is controversial. They are useful in high doses early in the reaction, but morbidity and mortality actually may increase in association with corticosteroid use.
Human intravenous immunoglobulin has been described as both treatment and prophylaxis. In the latter setting, one group used IVIG in a patient who underwent cardiac catheterization but who had 4 previous Stevens-Johnson syndrome (SJS) episodes after intravenous contrast injection.9
Follow-up
Further Inpatient Care
- Saline compresses may be applied to the eyelids, lips, and nose.
- Careful daily inspection is necessary to monitor for secondary superinfections.
- Prophylactic systemic antibiotics are not useful, especially in the current era of multiple-drug resistance.
- Antimicrobials are indicated in cases of urinary tract or cutaneous infections, either of which may lead to bacteremia.
Further Outpatient Care
- Although patients with erythema multiforme minor may be treated as outpatients with topical steroids, those with erythema multiforme major (ie, Stevens-Johnson syndrome) must be hospitalized.
- Cases of erythema multiforme minor must be followed closely. Some authors recommend daily follow-up.
Transfer
- Patients with Stevens-Johnson syndrome (SJS) are often critically ill; therefore, they must be admitted to hospitals capable of delivering critical care.
- Some patients may require the services of a burn unit.
- Transfer criteria would be the same as for patients with thermal burns.
Deterrence/Prevention
- Patients must avoid any future exposure to agent(s) implicated in the occurrence of Stevens-Johnson syndrome (SJS). Recurrences are possible.
Complications
- Ophthalmologic - Corneal ulceration, anterior uveitis, panophthalmitis, blindness
- Gastroenterologic - Esophageal strictures
- Genitourinary - Renal tubular necrosis, renal failure, penile scarring, vaginal stenosis
- Pulmonary - Tracheobronchial shedding with resultant respiratory failure
- Cutaneous - Scarring and cosmetic deformity, recurrences of infection through slow-healing ulcerations
Prognosis
- Individual lesions typically should heal within 1-2 weeks, unless secondary infection occurs. Most patients recover without sequelae.
- Development of serious sequelae, such as respiratory failure, renal failure, and blindness, determines prognosis in those affected.
- Up to 15% of all patients with Stevens-Johnson syndrome (SJS) die as a result of the condition.
- The SCORTEN score looks at a number of variables and uses them to prognosticate risk factors for death in both SJS and TEN. The variables include the following:
- Age >40 years
- Malignancy
- Heart rate >120
- Initial percentage of epidermal detachment >10%
- BUN level >10 mmol/L
- Serum glucose level >14 mmol/L
- Bicarbonate level <20 mmol/L
- Mortality rates are as follows:
- SCORTEN 0-1 >3.2%
- SCORTEN 2 >12.1%
- SCORTEN 3 >35.3%
- SCORTEN 4 >58.3%
- SCORTEN 5 or more >90%


My 12-year old daughter started breaking out in big open sores on her legs and arms over a 7-week period after starting Trileptal. We didn't make the connection until talking with our doctor again today, who suspects SJS. Waiting for a skin-punch biopsy she had done 4 days ago. She also has fever, fatigue, vomiting, and GERD-like symptoms - but it was confusing because her symptoms appeared only off-and-on. No more trileptal!
ReplyDeleteHi! nice post. Well what can I say is that these is an interesting and very informative topic. Thanks for sharing your ideas, its not just entertaining but also gives your reader knowledge.Cheers!
ReplyDelete- The Sevens-Johnson Syndrome
Thank you for visiting my blog.
ReplyDelete